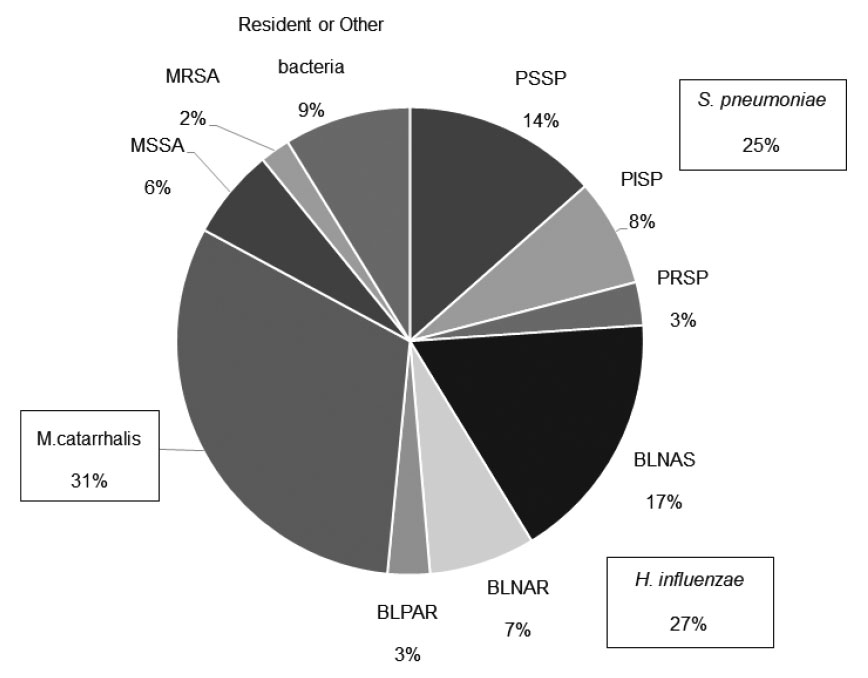
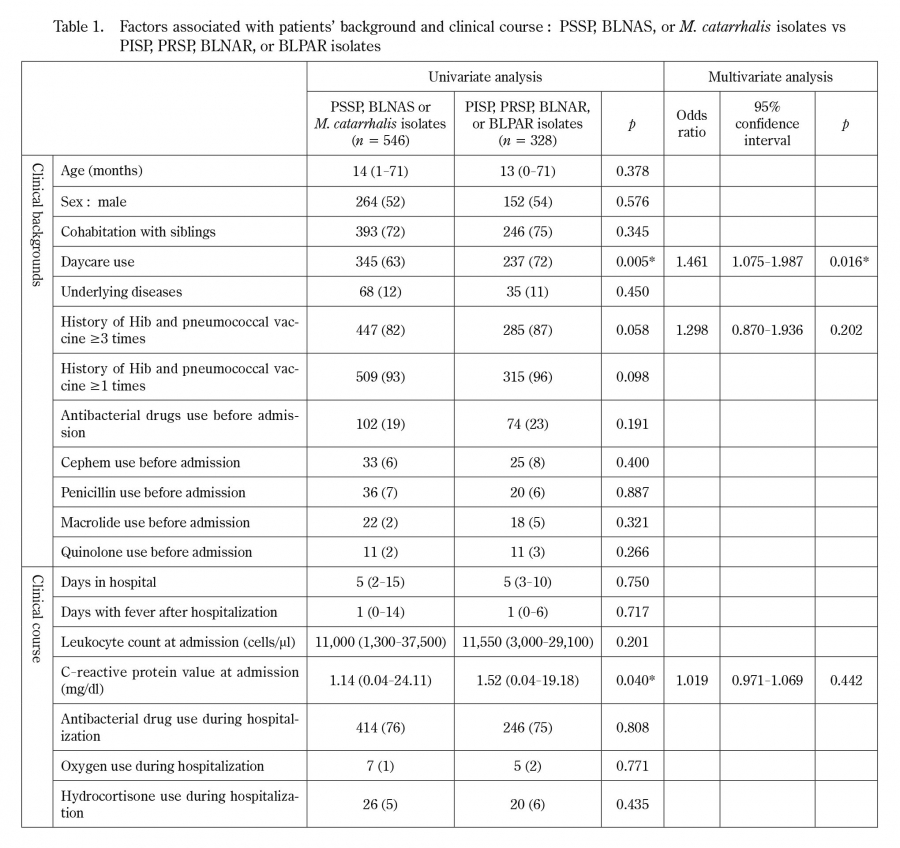
AbstractWe investigated the nasopharyngeal microbiota in preschool patients hospitalized with lower respiratory tract infection to clarify the relationships between culturable nasopharyngeal bacteria and prognosis. From 2016 to 2018, nasopharyngeal culture was performed on inpatients under 6 years of age with a lower respiratory tract infection. Among the 1,056 study patients, 1,046 provided nasopharyngeal samples that yielded positive cultures, yielding 1,676 isolated strains. Streptococcus pneumoniae, Haemophilus influenzae, and Moraxella catarrhalis, were isolated in 25%, 27%, and 31% of the samples, respectively, and were the major causes of respiratory tract infection in these children. The only factor associated with the isolation of antibiotic-resistant strains from the nasopharynx was daycare attendance, which did not affect clinical severity, such as duration of fever and hospitalization. This study demonstrated that resistant bacteria in the nasopharynx did not affect the severity of lower respiratory tract infection and supports the use of narrow-spectrum antimicrobial agents in accordance with published guidelines when initiating therapy for pediatric patients with community-acquired pneumonia.
Abstract/References
Clinical course and background of nasopharyngeal antibiotic-resistant bacteria carriers among preschool children hospitalized for lower respiratory tract infection
Aya Takeyama, Kenta Suzuki, Masaki Ito, Masatoki Sato, Koichi Hashimoto, Masahiko Katayose, Mitsuaki Hosoya
-
Aya Takeyama
Department of Pediatrics, Public Soma General Hospital
-
Kenta Suzuki
Department of Pediatrics, School of Medicine, Fukushima Medical University
-
Masaki Ito
Department of Pediatrics, Public Soma General Hospital
-
Masatoki Sato
Department of Pediatrics, School of Medicine, Fukushima Medical University
-
Koichi Hashimoto
Department of Pediatrics, School of Medicine, Fukushima Medical University
-
Masahiko Katayose
Nanohana Kids Clinic
-
Mitsuaki Hosoya
Department of Pediatrics, School of Medicine, Fukushima Medical University
Abstract
References
1. Sectish TC, Prober CG. Pneumonia. In: Kriegman Rm, Behrman RE, eds. Nelson textbook of pediatrics. 18th ed. Saunders, Philadelphia, 1795-1800, 2007.
2. Nohynek H, Eskola J, Kleemola M, Jalonen E, Saikku P, Leinonen M. Bacterial antibody assays in the diagnosis of acute lower respiratory tract infection in children. Pediatr Infect Dis, 14:478-484, 1995.
3. Borges IC, Andrade DC, Vilas-Boas AL, et al. Detection of antibody responses against Streptococcus pneumoniae, Haemophilus influenzae, and Moraxella catarrhalis proteins in children with community-acquired pneumonia:effects of combining pneumococcal antigens, pre-existing antibody levels, sampling interval, age, and duration of illness. Eur J Clin Microbiol Infect Dis, 34:1551-1557, 2015.
4. Sasaki K, Sato E, Saitoh N, Komatsu A. Bacteriological investigation of nasopharyngeal culture in the pediatric department in our hospital. (in Japanese) Japanese Journal of Medical Technology, 59:1292-1296, 2010.
10. Faden H, Duffy L, Wasielewski R, Wolf J, Krystofik D, Tung Y. Relationship between nasopharyngeal colonization and the development of otitis media in children. J Infect dis, 175:140-145, 1997.
13. Marik PE. Aspiration pneumonitis and aspiration pneumonia. N Engl J Med, 344:665-671, 2001.
14. Teo SM, Tang HHF, Mok D, et al. Airway Microbiota Dynamics Uncover a Critical Window for Interplay of Pathogenic Bacteria and Allergy in Childhood Respiratory Disease. Cell Host Microbe, 24:341-352, 2018.
16. Bosch AATM, de Steenhuijsen Piters WAA, van Houten MA, et al. Maturation of the Infant Respiratory Microbiota, Environmental Drivers, and Health Consequences. A Prospective Cohort Study. Am J Respir Crit Care Med, 196:1582-1590, 2017.
19. Tenenbaum T, Franz A, Neuhausen N, et al. Clinical characteristics of children with lower respiratory tract infections are dependent on the carriage of specific pathogens in the nasopharynx. Eur J Clin Microbiol Infect Dis, 31:3173-3182, 2012.
Figures (2)